
Everything You Need to Know About Being a Neonatal Nurse
As a neonatal nurse, you play a pivotal role in providing specialized care to newborns who require intensive medical attention. From premature infants to those born with health complications, your expertise and compassion are essential in ensuring these delicate patients receive the best possible care. Whether you’re a seasoned neonatal nurse or just starting out in this career field, this blog is packed with valuable information to help you succeed. Let’s dive in and explore the world of neonatal nursing together!
What is a Neonatal Nurse?
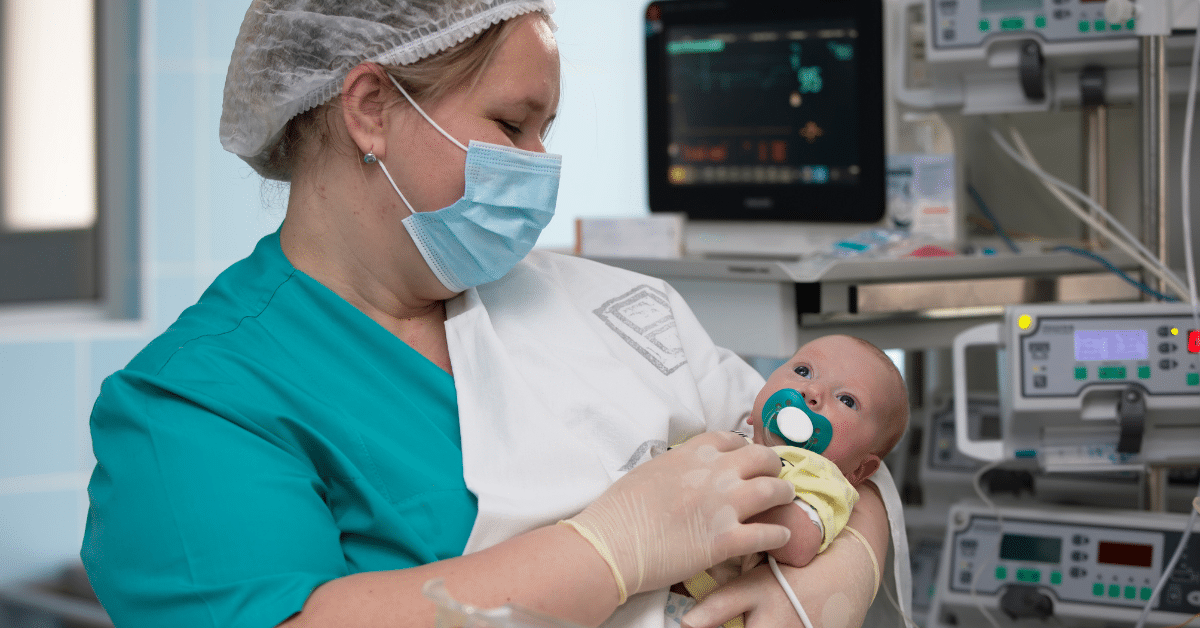
A neonatal nurse is a specialized healthcare provider who cares for newborn infants, particularly those who are born prematurely, with medical conditions, or in need of intensive medical attention. These dedicated professionals work closely with medical teams to deliver specialized treatments and interventions that help these vulnerable infants overcome challenges and thrive. Neonatal nurses possess a unique blend of compassion and expertise, which allows them to provide not only medical care but also emotional support to both the tiny patients and their anxious families during the critical early stages of life.
Neonatal Nurse Responsibilities
A neonatal nurses responsibilities encompass a wide range of tasks, including:
- Monitoring vital signs and symptoms: Neonatal nurses are responsible for monitoring the vital signs and symptoms of newborns, including heart rate, breathing, and blood pressure. They use specialized equipment to track these signs and look for any changes that could indicate a problem.
- Administering medication: Neonatal nurses may be responsible for administering medication to newborns, including antibiotics, pain medication, and nutrition through IVs or feeding tubes. They must ensure that the correct dosage is given, and the medication is delivered safely.
- Assessing newborns: They perform thorough assessments of newborns, evaluating their physical condition, neurological responses, reflexes, and overall development. Any abnormalities or concerns are promptly reported to the medical team.
- Feeding and nutrition: Neonatal nurses work with parents and doctors to develop feeding plans for newborns, including providing breastmilk or formula through a feeding tube. They monitor the baby’s weight and growth to ensure that they are getting enough nutrition.
- Bathing and changing: Neonatal nurses are responsible for the basic care of newborns, including bathing, changing diapers, and keeping them clean and comfortable,
- Educating parents: Neonatal nurses play an important role in educating parents about how to care for their newborns, including breastfeeding, safe sleep practices, and recognizing signs of illness.
- Assisting with medical procedures: Neonatal nurses may be responsible for assisting doctors with medical procedures, including intubation, central line placement, and surgeries.
- Emergency Response: In critical situations, neonatal nurses are trained to respond quickly and effectively to emergencies, such as respiratory distress or cardiac arrest, administering life-saving interventions.
- Emotional support: Neonatal nurses provide emotional support to parents and families, who may be going through a difficult time. They offer guidance and counseling to help families cope with the stress of having a sick or premature baby.
- Discharge planning: As infants improve and prepare to go home, neonatal nurses assist with discharge planning, educating parents about ongoing care, follow-up appointments, and necessary resources.
Overall, these nurses play a critical role in the care of newborns and their families, providing medical care, emotional support, and education to ensure the best possible outcomes for these tiny patients.
Benefits of Being a Neonatal Nurse
The decision to become a neonatal nurse comes with numerous rewards:
Making a Meaningful Impact: Neonatal nurses have the privilege of contributing to the successful recovery and growth of fragile infants, leaving an permanent mark on their lives and the lives of their families.
Skill Advancement: This field offers the opportunity to acquire advanced clinical skills in handling neonatal patients, from assessing their health status to delivering precise interventions.
Job Satisfaction: The emotional fulfillment derived from seeing tiny patients overcome obstacles and grow stronger is immeasurable.
Career Growth: Experienced neonatal nurses can explore avenues such as becoming nurse practitioners, clinical nurse specialists, or educators within the neonatal field.
Required Education for Neonatal Nurses
Embarking on a journey as a neonatal nurse involves several educational steps:
Nursing Education: Begin with an associate or bachelor’s degree in nursing from an accredited institution. This forms the foundation of nursing knowledge and skills.
Nursing Licensure: Pass the National Council Licensure Examination for Registered Nurses (NCLEX-RN) to become a licensed registered nurse.
Clinical Experience: Acquire practical experience by working in settings like labor and delivery, pediatrics, or maternity wards.
Specialized Training: Some nurses pursue additional certifications like the Neonatal Resuscitation Program (NRP) or Neonatal Intensive Care Nursing Certification (RNC-NIC) to enhance their expertise.
Qualities of a Good Neonatal Nurse
Successful neonatal nurses possess specific qualities that enable them to excel in this demanding profession:
- Compassion: A deep empathy for infants and their families, helping them navigate challenging circumstances.
- Attention to Detail: Precision is paramount when administering medications, performing procedures, and monitoring fragile patients.
- Critical Thinking: The ability to assess situations swiftly and accurately, making informed decisions in high-pressure environments.
- Communication Skills: Clear communication with medical teams and families ensures seamless patient care and emotional support.
Levels of Neonatal Nursing
Neonatal nursing is categorized into three levels, each with unique characteristics:
Level I:
Level 1 neonatal nurses possess a diverse skill set that includes proficiency in neonatal resuscitation, comprehensive well-care for newborns, and specialized attention to babies born at 35-37 weeks of gestation. They also play a vital role in the stabilization of infants born at less than 35 weeks of gestation, offering essential care until the point of transfer to higher levels of care. In the context of neonatal nursing’s different tiers, Level 1 nurses serve as the foundation of support, ensuring that healthy newborns receive optimal care and aiding parents in establishing breastfeeding routines. Their expertise in routine assessments and early interventions contributes significantly to the healthy development of newborns during their critical early days.
Level II:
Level II neonatal nurses stand as invaluable caregivers for infants born at 32 weeks gestation, expertly supporting their crucial developmental phase. Proficient in tasks ranging from mechanical ventilation to intravenous fluid administration, these nurses skillfully navigate the intricate care required by premature newborns. Their adeptness extends to specialized feeding techniques, oxygen therapy, and other essential interventions that bridge the gap between medical necessity and compassionate support. Whether it’s aiding the transition from assisted to independent breathing or managing issues like jaundice through phototherapy and nasogastric feeding, Level II neonatal nurses play a pivotal role in nurturing these vulnerable infants during their early stages of life.
Level III:
Level III neonatal nurses excel in the neonatal intensive care unit (NICU), where they provide specialized care to profoundly ill newborns. These infants, often born prematurely or with complex medical conditions, require meticulous attention. Equipped with expertise in utilizing vital equipment like incubators and ventilators, these nurses play a pivotal role in ensuring the stability of infants who may need surgical interventions and continuous life support. From managing low birth weights to collaborating with specialists, Level III neonatal nurses demonstrate exceptional vigilance and compassion as they monitor and enhance the well-being of these vulnerable patients.
Neonatal Nurse Earnings, Workplaces, and Job Outlook
Neonatal nurses are rewarded with competitive salaries that vary according to factors such as location, experience, and education. These devoted professionals predominantly serve within the neonatal intensive care units (NICUs) nestled within hospitals. Beyond this, avenues also extend to pediatric clinics, research institutions, and even home healthcare settings. As neonatal medicine thrives with advancements, and premature infants’ survival rates surge, the future for neonatal nurses gleams with promise due to the ever-present requirement for specialized care.
Based on insights from PayScale data in August 2023, neonatal nurses can anticipate earning an approximate $71,989. It’s noteworthy that as a travel nurse, you can expect even greater financial rewards, as travel nursing offers the opportunity to earn higher salaries, benefit from various incentives, and experience new environments while delivering your expert care.
Neonatal nursing is a field of unwavering dedication, expertise, and compassion. It demands a unique blend of clinical skills and emotional resilience. By choosing to become a neonatal nurse, you embark on a journey that impacts lives in ways that words cannot fully express. The opportunity to care for these precious lives during their earliest and most vulnerable moments is a privilege that defines the essence of neonatal nursing.
Please note that salary figures and job outlook details may vary and are influenced by external factors.
Take the next step in your career by applying for our available positions in the Neonatal Intensive Care Unit (NICU) today!
Share This Article
Similar Blogs
The Role of Staffing Agencies in Addressing the Nursing Shortage
The nursing shortage has become a critical challenge for healthcare facilities across the United States, putting immense pressure on patient care and healthcare delivery. Staffing agencies like TheraEx…
Posted: 2 Days Ago
Mental Health for Healthcare Professionals During the Holiday Season
The holiday season can be a challenging time for healthcare professionals. While many people enjoy celebrations and time off, healthcare workers often face increased workloads, holiday shifts, and…
Posted: 2 Days Ago
Holiday Travel Tips for Healthcare Workers
The holiday season is a magical time of year, but for healthcare workers, balancing work responsibilities with holiday travel can be a challenge. With demanding schedules, unexpected shifts,…
Posted: 2 Days Ago


